Some Miscellaneous Tidbits About Shock
Hypovolemic Shock
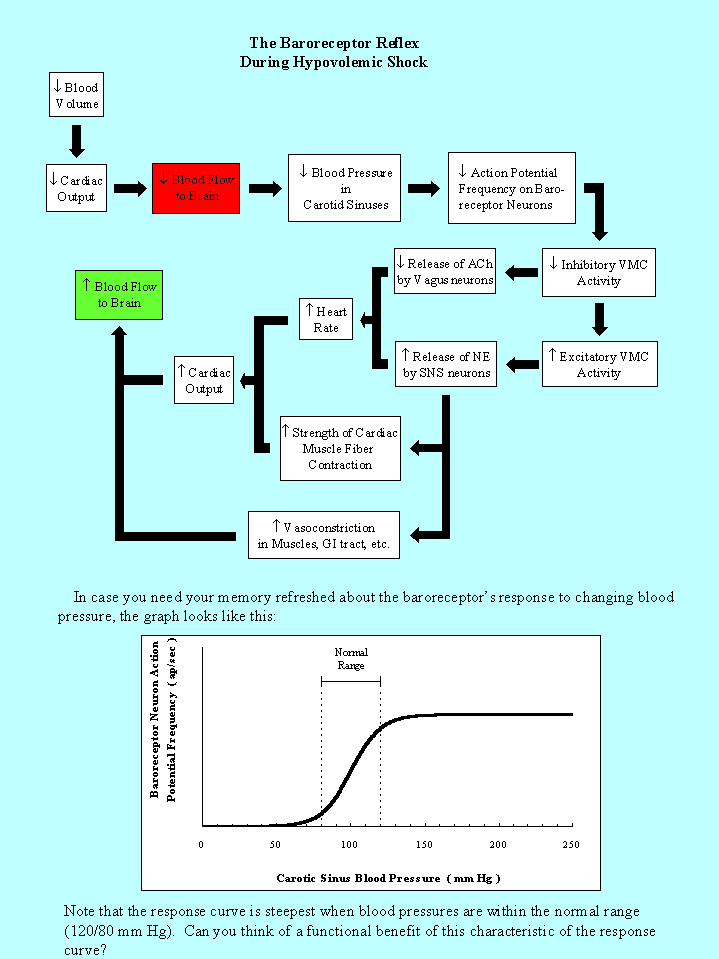
Normal Cardiovascular System Response To Hypovolemic Shock
You will also be able to use the above diagram to 'walk your way through' the response of the baroreceptor reflex to virtually any situation involving a response of the cardiovascular system.
Neurogenic Shock
Irreversible Shock
What Else Does The Baroreceptor Reflex Do For Us?
Perhaps the easiest form of shock to understand is the one that develops when the volume of blood in the circulatory system falls below normal limits. If the volume of blood in the cardiovascular system is reduced, there will be less blood for the heart to pump. If the reduction in blood volume is great enough, cardiac output may be reduced enough to put a person into shock. Because this form of shock is the result of an abnormally low blood volume, it is termed hypovolemic shock. There are several ways for hypovolemic shock to be induced, some of which are obvious, some of which will probably surprise you.
Hemorrhagic Shock
Probably the most obvious cause of hypovolemic shock is loss of blood, which is termed hemorrhagic shock. A serious wound, especially one that severs a large artery, can result in loss of sufficient blood to cause shock.
However, such loss of blood from the body, while readily perceived and therefore treated, is not the only way for hemorrhagic shock to develop. Loss of blood from the cardiovascular system can occur internally, as well as externally. For example, hypovolemic shock is a serious risk following blunt force trauma to the chest or abdomen. Emergency-room personnel know that they must carefully assess for internal bleeding anyone who has suffered a blow to the abdomen or chest as a result of, say, a bicycle or motorcycle accident. This is because the force of the blow can rupture the aorta, spleen, or liver, and __ even in the absence of any apparent external injuries or symptoms __ result in severe internal bleeding which can easily induce a state of potentially fatal hypovolemia and shock. You will perhaps recall the unfortunate professional bull rider who died here in Albuquerque a couple months ago after being stepped on by a bull. His death almost certainly resulted from internal bleeding and shock subsequent to rupture of one of the organs mentioned above.
Hypovolemia sufficient to induce shock can also accompany a blocked intestine. This may be surprising to you, since it might seem that a blockage of the intestine would not be a serious problem unless it persisted for a prolonged interval. However, any of you who have had a horse or cat that suffered an intestinal blockage know that this is a serious surgical emergency that requires immediate treatment. That's true for humans, too. The problem is that the blocked intestine rapidly becomes distended and stretches the tissues that form the intestinal wall. This stretching causes damage to the microcirculation components, which respond by becoming leaky to fluids. The resulting rapid loss of fluid from the blood stream into the lumen of the (plugged) intestine can very rapidly produce hypovolemia and lead to shock within a few hours.
Other Causes Of Hypovolemic Shock
A reduction in blood volume sufficient to cause shock can occur in other ways that don't involve hemorrhage, per se. For example, dehydration resulting from any number of causes can reduce the blood volume enough to induce hypovolemic shock.
Vomiting and/or diarrhea, particularly in infants, can quickly result in dangerous degrees of dehydration. In fact, this is why cholera is such a deadly disease. The cholera bacterium, to facilitate its spread to other hosts, produces a toxin that does nothing more than make the capillaries of the intestinal tract lining highly permeable to water. This results in massive efflux of water from the blood into the lumen of the intestine which, in turn, induces severe diarrhea. The resulting water losses are so rapid that it's very difficult to replace them quickly enough to prevent death due to dehydration-induced hypovolemic shock. In fact, cholera patients have been successfully treated by having them drink large volumes of Gatoradeä!
Severe burns, because they destroy the waterproofing layers of the skin, often result in such rapid evaporation of water from the tissues and blood that the victim can die of dehydration-induced circulatory collapse (shock) within a few hours. Replacing the fluids lost to evaporation is one of the most critical __ and difficult __ problems that must be solved during the treatment of burn victims, and many such unfortunate persons die due to this cause alone.
Finally, other bacterial toxins, particularly those produced by certain strains of Staphylococcus or Streptococcus, can cause the capillaries to become so leaky to fluid that a huge proportion of the plasma (the liquid fraction of the blood) leaks out of the blood stream and into the intercellular spaces, where it's no longer available to the cardiovascular system for circulation. The resulting hypovolemic shock (termed toxic shock) can result in rapid organ damage and even death, in part because there's insufficient volume of blood to maintain adequate blood flow even to the brain, in spite of the baroreceptors' best efforts.
The flow diagram below will take you step-by-step through the response of the baroreceptors to hypovolemic shock. Follow through the steps, making sure that you understand exactly what occurred to produce the response indicated in each box.
As the name implies, this form of shock involves the nervous system. The basic cause of neurogenic shock is massive inhibition of both the Excitatory and Inhibitory portions of the Vasomotor Center. Now, you might think that 'simply' inhibiting the Vasomotor Center would not be too big a deal.....that inhibition of the Inhibitory Portion would result in a small increase in heart rate and cardiac output, while inhibition of the Excitatory Portion would probably cause a small decrease in cardiac output. With both parts being shut down simultaneously, you might predict little or no change in cardiac output. In fact, there's usually a small decrease in cardiac output, so you might wonder, "What's the problem"?
Well, the problem is that inhibition of the Excitatory Portion of the Vasomotor Center also results in vasodilation throughout the body, due to inactivation of the tonic vasoconstrictor neurons that are normally being stimulated by the Excitatory Vasomotor Center. This vasodilation, coupled with the decreased cardiac output, typically results in a drastic reduction in blood flow to the brain, a reduction sufficient to lead to damage within a relatively short time.
The two principal causes of neurogenic shock are trauma to the medulla (say, from a head injury) and general anesthetics. The first cause is pretty self-explanatory, but the second merits some discussion. Most general anesthetics work because they target parts of the medulla oblongata that are involved in keeping us awake and alert. These portions of the medulla __ part of the Reticular Activating System (RAS)__ send action potentials to higher brain centers (such as the frontal cortex). These action potentials stimulate the portions of the brain to which they are transmitted, and these stimulated brain centers' activity is what keeps us awake. General anesthetics block the medullary portions of the RAS, and thus prevent them from generating the action potentials that ultimately activate the higher brain centers. The forced inactivity of the higher brain centers is what causes us to lose consciousness.
However, because the general anesthetic is targeting the medulla, it can also inhibit both the Excitatory and Inhibitory Vasomotor Center. That inhibition can result in neurogenic shock. Obviously there are interindividual differences among people with respect to their susceptibility to anesthetic-induced neurogenic shock, and considerable research is done in development, testing, and risk-assessment before a chemical agent is approved for use as an anesthetic agent. However, as any of you who have had surgery involving a general anesthetic (or have know someone who did) are aware, blood pressure is carefully monitored during surgery and the post-operative recovery period. Now you know why!
The problem with trying to treat neurogenic shock is that the baroreceptor reflex can't help maintain adequate blood flow to the brain, because the Vasomotor Center isn't functioning and therefore can't increase cardiac output or even shunt blood away from other, less O2-sensitive, organs and route it to the brain. This makes neurogenic shock a serious emergency calling for aggressive treatment.
All of the forms of shock mentioned above are potentially lethal __ even if adequate blood flow to the brain is maintained, either by the baroreceptor reflex or by medical procedures __ because of a phenomenon known as irreversible shock. If, for example, hemorrhagic shock __ no matter how it's induced __ is severe enough, the baroreceptor reflex can be powerful enough to reduce blood supply to the other tissues/organs to levels below the minimum that they need to survive. Neurogenic shock is even more of a threat, because the baroreceptor reflex can't function to increase cardiac output. Either way, deep shock, if not treated successfully within about 24 hours can result in such severe damage to sensitive organs that they cease functioning. Then, even if the patient recovers from the initial cause of the shock, death from failure of the kidneys or other organs such as those that comprise the gastrointestinal system is a probable outcome.
Hopefully you will never experience true physiological shock, and hopefully you will only rarely experience extreme episodes of the Hypothalamic Alarm Reaction that we discussed in lecture. However, you still want to be nice to your Baroreceptor Reflex, because it actually works day-to-day, minute-to-minute, second-to-second to make sure that blood flow to the brain and the pressure of blood reaching the brain are kept within homeostatic limits.
Let's say you're standing or sitting in a upright posture. In this position, your heart is a considerable distance below your brain, and the natural tendency of the blood leaving the left ventricle is to flow downward, away from the brain, and extra 'effort' is required to get blood to the brain. Under this circumstance, your Excitatory VMC is a little extra active (can you tell me why?), and both cardiac output and peripheral vasoconstriction are consequently a bit elevated (by about 25-50%). These two 'events' result in adequate brain blood flow.
Ok, let's have you lie down. Now, your brain is at the same level as your heart, and it becomes easier for the heart to get blood to it. If the heart continues to pump as strongly as when you were standing __ and if peripheral vasoconstriction is maintained to the same degree __ there will be too much blood being sent towards the brain, and its pressure will be too high. This is potentially a very dangerous situation because if the volume and/or pressure of blood reaching the brain are too great, too much fluid will leak through the capillary walls into the brain's extracellular fluid compartment.
The presence of extra fluid in the extracellular fluid compartment of any part of the body is termed edema, and in the brain, we call it cerebral edema. (swollen feet after prolonged standing are an example of edema, as is the swelling of injured tissues, such as a sprained ankle, the edges of a cut or scratch, etc.). Cerebral edema is a real no-no, and can result in symptoms ranging from sensory disturbances and headache (the terrible pain associated with migraine headaches is mostly the result of cerebral edema, for example) to unconsciousness. In extreme cases of cerebral edema, which can accompany a severe head wound, brain damage or even death can result.
Well, when you lie down, the pressure in your carotid sinuses increases and your baroreceptor reflex kicks in to bring it back down (can you use the above diagram to explain how this happens?). The response to postural changes (standing, sitting, lying down, kneeling, etc.) is probably the single most important function of the baroreceptor reflex during your life span. That's why I urge you to be nice to it………