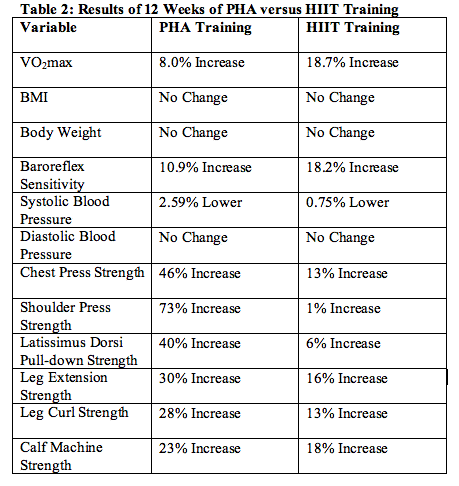
| Peripheral Heart Action Training: "What's Old is New Again" Len Kravitz, Ph.D. Study Reviewed Study Reviewed: Piras, A., Persiani, M., Damiani, N. et al. (2015). Peripheral heart action (PHA) training as a valid substitute to high intensity interval training to improve resting cardiovascular changes and autonomic adaptation. European Journal of Applied Physiology, 115, 763-773. Introduction Peripheral heart action (PHA) training is a system of conditioning developed by Dr. Arthur Steinhaus in the 1940's (Piras et al., 2015). The concept of this training is to keep blood consistently circulating during the resistance training session. Five to six exercises are performed sequentially (and with no rest between exercises) at a medium-intensity to alternately stress the upper and lower body muscles (Piras et al.). Interestingly, despite the early introduction of PHA to the fitness world, very little investigation has been conducted to examine its effect on cardiovascular and autonomic function (branch of nervous system that controls internal organs and regulates heart rate, respiration and cardiac function). Recently, Piras and colleagues compared the cardiovascular and autonomic function effect of PHA to high intensity interval training in a young, untrained population. Study Subjects Eighteen healthy volunteers (9 women and 9 men, 24yrs, BMI=22.67) were randomly assigned to a HIIT group (8 subjects) or a PHR group (10 subjects). All participants were disease-free non-smokers, not on any prescribed medications. The participants were recreationally active, but untrained, and their maximal aerobic capacity average was 32.89 ml/kg/min, which is a 'poor' classification for their age and gender. Study Methods All volunteers did a pre and post-test within 3-4 days of a 3-month training period consisting of three sessions per week of exercise, each day separated by 1-2 days of rest. All training sessions were supervised by one of the study researchers. Muscular strength was assessed with 1-RM testing of the pectoralis major and minor, quadriceps, latissiums dorsi, hamstrings, deltoids, hamstrings and gastrocnemius. Autonomic function was measured with heart rate variability (the physiological variation in the time interval between heartbeats) and baroreflex sensitivity (a measure of the interaction between sympathetic and parasympathetic activities that directly affect cardiac health). HIIT Training Group For the HIIT training, the subjects completed a 5-min warm-up on a cycle ergometer and began the HIIT training with a 1-min high intensity work bout at the level of their maximal aerobic capacity. This was followed by a 2-minute (no load on the cycle) recovery cycle interval. The work and recovery intervals were repeated 5 times with a 5-min cool-down at the end of the workout. PHA Training Group Each PHA session began with a 5-min warm-up and concluded with a 5-min cool-down. The PHA consisted of 6 exercises strictly ordered in this circuit sequence: pectoralis major, leg extension, latissimus dorsi pull-down, leg curl, shoulder press and calf machine (See Figure 1). There was no rest between exercises. All subjects completed 15 repetitions for each exercise that was at 55-60% of their 1-repetition maximum (1-RM). After the completion of one circuit the subjects rested 1 minute and then complete another circuit in the precisely same fashion until a total of 4 circuits were completed. Subjects also wore heart rate monitors during the PHA training. Heart rates were held consistently during the PHA training at 60-80% of their maximal heart rate (calculated from their maximal aerobic capacity pre-test). Table 1: Exercises Performed in this Order Bench Press Len Extension Latissimus dorsi pull-down Leg Curl Shoulder Press Seated Heel Raise Note: Men and women participants did 15 repetitions (55-60% of 1-RM) of each exercise with no rest between exercises. After completing a circuit subjects rested 1 minute and then continued to complete a total of 4 circuits. Study Results This is the first longitudinal 12-week study to complete such an exhaustive analysis of PHA training, as compared to HIIT training. Table 2 synthesizes many of the study results. Most interestingly, the improvement in maximal aerobic capacity for PHA is higher than that reported in traditional circuit training studies. The PHA concept of alternating upper and lower body exercises, performed at a medium exercise intensity (with no rest between exercises), stimulates several variables of cardiovascular function. Piras and colleagues hypothesize that PHA training appears to provide the appropriate stress for the cardiovascular system to adapt. The researchers believe that PHA training may likely have a beneficial effect on peripheral blood flow (i.e. in the arms, hands, legs and feet) during the training as well as improving cellular metabolic activity. With PHA, the heart rate variability makers of autonomic activity (controlling heart rate) were reduced for the sympathetic modulation and increased for the vagal modulation. These results indicate a very positive response for improving cardiac control, and they were more favorable in the PHA group (as compared to the HIIT group). The baroreflex sensitivity markers showed equal improvement in the 12-week study for the PHA and HIIT training groups. As expected, the PHA training group showed much better muscular strength improvements in the lower body and upper body musculature. Piras et al. (2015) highlight the importance of these findings may be most beneficial in the prevention or management of metabolic syndrome, obesity, sarcopenia and osteoporosis. After 12 weeks of training, PHA training showed meaningful lower systolic blood pressure changes that were greater than the HIIT training. Piras et al. (2015) propose that PHA training should be considered as a viable option for persons with elevated blood pressure or with clinical pathology health conditions that do not allow them to train at high intensities. Piras continue that combining HIIT training with PHA may very likely even have greater benefits when it comes to reducing elevated blood pressure in persons with hypertension. Is There a Physiological Mechanism at Work with PHA Training? There is no rest between sets with PHA, and the exercises alternate between upper body and lower body. In 1978, Asumusen and Maxin showed the more dynamic exercise work can be accomplished by exercising continuously between different muscle groups as compared to providing a rest between the exercises. Piras et al. (2015) propose that this continuous increase in blood flow during the PHA training session may very likely be more effective in removing the metabolites (i.e., hydrogen ions and carbon dioxide) that contribute to fatigue. What's Old is New Again The results of this study are most impressive. PHA training promotes positive adaptations to several variables or cardiovascular function, blood pressure and autonomic regulation. The improvements in heart rate variability and barometric sensitivity are associated with lowered risk to all causes of mortality and morbidity. All of these improvements translate into greater cardioprotection from cardiovascular disease. In addition, the muscular strength benefits of this type of training are quite impressive. What's old is new again, and this new, promising PHA research suggests this type of training is going to be around for quite some time. @bio:Len Kravitz, PhD, CSCS is the program coordinator of exercise science and a researcher at the University of New Mexico, Albuquerque, where he won the Outstanding Teacher of the Year award. He has received the prestigious Can-Fit-Pro Lifetime Achievement Award and American Council on Exercise Fitness Educator of the Year. Additional Reference: Asmussen E., and Mazin, B. (1978). Recuperation after muscular fatigue by “diverting activities”. European Journal of Applied Physiology and Occupational Physiology, 38:1-7 |
||||||||
 |
||||||||
|
|
||||||||
|