| Metabolic Effects of Resistance Training Zachary Mang, M.S., Amber L. Logan, Fabiano T. Amorim, PhD and Len Kravitz, PhD Introduction The benefits of resistance training (RT) for improving muscular strength, muscular endurance and bone mineral density and mass are well-established. Several studies within the last few years are now revealing some impressive metabolic (i.e., related to metabolism) findings with RT in the management and or prevention of type 2 diabetes, high blood pressure, obesity, and high cholesterol levels, as well as for the improvement of resting metabolic rate and cardiorespiratory fitenss. The pendulum has definitely shifted from the original touted benefits of RT to the point that some authors are starting to call it an exercise therapy program (Strasser & Schobersberger 2011). A synthesis of the major metabolic effects of RT presented in this article confirm these new viewpoints. As well, the proposed mechanisms leading to these positive changes are discussed. Diabetes Background Information Diabetes mellitus is a common metabolic disorder in which a person either does not produce insulin (type 1 diabetes) or does not respond well to insulin (type 2 diabetes). An estimated 30.3 million people have diabetes, which is 9.4% of the U.S. population (CDC 2017). Type 2 diabetes (T2D) accounts for approximately 90-95% of all diabetes cases (CDC 2017). According to 2015 data, 33.9% of U.S. adults aged 18 years or older (or 84.1 million people) have prediabetes based on their fasting glucose (100 to 125 mg/dL) or A1C (5.7% to 6.4%) levels. As people age, so does the prevalence (widespread presence) of T2D. Data indicate that 25.2% of person's 65 or older have diabetes (CDC 2017). Resistance Training Research in Diabetes Populations A 10-week study by Bweir and colleagues (2009) compared the effects of RT vs. aerobic training (AT) on blood glucose and A1c levels in 20 inactive male and female participants (ave age = 53 years) with T2D. The aerobic group progressed from 20 minutes, at 60% of their maximum heart rate (HRmax) to 30 minutes, at 75% HRmax during the course of the study. The RT group performed 3 sets of 8-12 repetitions for 7 exercises (including knee and hip flexion/extension, shoulder flexion/extension, shoulder adduction/abduction, elbow flexion/extension and a chest press). After the intervention, the RT group experienced an impressive, and more favorable decrease (-18%) in A1c compared to the AT group (-8%). Yavari and colleagues (2012) compared the effects of RT alone, aerobic training (AT) alone, or combined (CT) RT + AT in 80 obese participants (37 men and 43 women) with T2D in a year long study. The participants were divided evenly into 4 groups and did the following training protocols. The AT group trained on treadmills, ellipticals or stationary bicycles, progressing from 20 to 60 minutes at 60-75% HRmax, on three non-consecutive days/week. The RT group started training with 2 days per week during the first month and increased to 3 non-consecutive days per week for the remainder of the study. The RT group initially trained 1-2 sets (first month) at 60% one repetition max (1RM) and progressed to 3 sets of 8-10 repetitions at 75% 1RM on 10 different upper body and lower body exercises. The CT group did the AT plus the RT programs on 3 days of the week. After 52-weeks the A1c values favorably decreased by 1.33%, 0.55%, and 1.74% in the AT, RT, and CT training groups, respectively. The authors note that previous research suggests that a reduction of A1C of .66% is considered a very good marker for improved glycemic control. The control group had an unfavorable 0.2% elevation in A1c. Yavari et al. submit that combing RT and AT clearly shows an additive effect in the prevention or management of T2D, thus a blend of exercise modalities is highly recommended for clients with T2D. How does RT Help Prevent or Manage T2D? It is proposed that RT improves glucose clearance and insulin sensitivity by increasing the concentration, activity, and/or sensitivity of GLUT4, insulin receptors, protein kinase B beta, and glycogen synthase (Holten et al., 2004). The GLUT4, insulin receptors and protein kinase B beta are proteins all involved in glucose transport into the muscle cell for energy. Glycogen synthase is involved in converting glucose molecules into stored glycogen in the muscle (to be eventually used for energy needs). Also, an increase in lean mass from RT may contribute to reduced visceral adipose tissue (Stasser and Schobersberger, 2011). By contrast, Strasser and Schobersberger note that a loss of muscle mass has been shown to lead to an increased risk for the development of obesity-associated insulin resistance and type 2 diabetes mellitus. Importantly, RT has been shown to decrease A1C levels in diabetic women and men, regardless of age. Practical Recommendations The American Diabetes Association position statement (Colberg et al., 2016) recommends that persons initially complete 1-3 sets of 8 to 10 exercises (total body), performing 10-15 repetitions for each exercise until near failure. Progress to a moderate intensity where no more than 15 repetitions can be performed with each set. For a vigorous RT program, perform 6-8 repetitions per exercise to failure (i.e., not able to perform any more repetitions). Complete the RT on a minimum of 2 and preferable 3 days per week. Colberg and colleagues recommend that a favorable progression is to initially increase loads (i.e., progression from 10-15 repetitions to 6-8 repetitions to failure) followed by an increase in sets (up to 3 sets) and then an increase in frequency (from 2 to 3 days per week). Blood Pressure Background Information The American Heart Association (AHA, 2017) defines blood pressure as the force of blood exerted against vessel walls during heart contraction (systolic blood pressure; SBP) and relaxation (diastolic blood pressure; DBP). Normal blood pressure is defined as SBP of <120 mmHg and DBP of <80 mmHg; pre-hypertension is defined as SBP >120-139 and DBP >80-90 mmHg; and high blood pressure (HBP: i.e., hypertension) is defined by SBP > 140 mmHg and/or DBP > 90 mmHg (AHA, 2017). It is estimated that 80.0 million adults &Mac179;20 years of age have HBP (Mozaffarian et al, 2015), which is a major risk factor for heart disease and stroke. Mozaffarian and colleagues add that HBP is on the rise with an estimation that 41.4% of adults will have HBP in 2030. Mozaffarian et al. continue that many markers (several modifiable) for the development of hypertension include ethnicity, age, overweight, physical inactivity, tobacco use, sleep apnea, family history of hypertension and genetic factors, and dietary factors (e.g., higher sodium intake, dietary fats, excessive alcohol intake, and low potassium intake). Resistance Training Research in Hypertensive Populations A monumental study by Westcott and colleagues (2009) evaluated the dose-response relationship between RT exercise and changes in BP. For 10 weeks, 1619 untrained and sedentary participants (77% women, 23% men, 21-80 years old) exercised either 1, 2 or 3 sessions/week). Each session consisted of 20 minutes of aerobic training (70-80% age-predicted maximum heart rate; <15 RPE) and 20 minutes of RT (1 set; 8-12 repetitions to volitional fatigue; 10 total body exercises). On average, SBP decreased by 3.83 mmHg, and DBP decreased by 1.73 mmHg. Westcott and colleagues highlight that 2 or 3 sessions a week of training appears to elicit the most beneficial influence on managing or lowering blood pressure (when elevated). Research by Piras and colleagues (2014) used Peripheral Heart Action (PHA) training to provide evidence that RT can reduce BP directly. With PHA training, participants sequentially alternate upper body and lower body exercises in a circuit (see IFJ, volume 13, issue 5 for a review of PHA). This type of training is theorized to enhance blood flow through the body during the training. Subjects performed 4-rounds of circuit resistance training (15 repetitions at 55-60% 1-RM) in the following order: chest press, leg extension, latissimus dorsi pull down, hamstring curl, shoulder press, and heel raises (note the alternating upper and lower body sequence). There was no rest between sets and only 1-minute of rest between each completed circuit. After 30 training sessions, exercising 3 nonconsecutive days/week, over the course of 3 months, the PHA participants significantly reduced their systolic (-2.59 mmHg) and mean arterial blood pressure (-1.69 mmHg). Mean arterial blood pressure is the average blood pressure in a person's arteries during one heart beat. These results corroborate research review results observed by Cornelissen and Smart (2013), who analyzed 93 studies and concluded that RT significantly reduces SBP (-1.8 mmHg) and DBP (-3.2 mmHg). How Does RT Help Prevent or Manage High Blood Pressure? Although the preponderance of research on exercise and blood pressure has focused on the mechanisms how cardiovascular exercise improves blood pressure, there are some interesting findings with RT. For instance, Olson et al. (2006) examined the effects of 1 yr of RT on vascular structure and function in overweight, healthy women. The primary finding of the study was that RT alone favorably improved brachial artery endothelial function in this group of overweight women. The endothelium is a membrane on the inside of the blood vessels in the body and heart. The endothelial cells release substances that control blood vessel contraction, relaxation, blood clotting, and immune function. They are very involved in blood pressure regulation. In another study by Beck et al. (2013), with 18-35 yr old men and women diagnosed with prehypertension, an 8-week RT program (3 times/week) showed that resistance training positively reduces peripheral blood pressure (i.e, arms, hands, legs and feet), improves endothelial function, and enhances other blood vessel substances involved in the regulation of vascular tone (degree of constriction in blood vessels when fully open). Practical Recommendations For the safety of the pre-hypertensive and hypertensive client, and to improve endothelial function, de Sousa et al. (2017) suggest the intensity of resistance training should NOT be performed to concentric failure. A review of the studies in de Sousa's meta analysis show that programs eliciting positive results in lowering blood pressure (when elevated) have participants train 3 days/week at 40% to 80% of 1RM on 7-10 exercises (working the major muscles of the body). The participants progress up to 2-3 sets of 8-15 repetitions, with 60 to 180 seconds rest between sets. Resting Metabolic Rate and Excess Post-Exercise Oxygen Consumption Background Information Resting metabolic rate (RMR) is the largest component of total daily energy expenditure, accounting for 50-75% of daily caloric expenditure (Aristizabal et al. 2015). It is the caloric expenditure required to keep the body functioning at rest. Excess post-exercise oxygen consumption (E.P.O.C) is the increased rate of oxygen uptake following dynamic exercise. Specifically, E.P.O.C. represents the energy required to restore the body to its pre-exercise condition. Both RMR and E.P.O.C. are somewhat similar physiological measures of energy expenditure of the body that we have combined in this section. Resistance Training Research with RMR and E.P.O.C. Aristizabal et al. (2015) recruited 61 recreationally active women and man aged 18 to 35 years, who had not resistance-trained for a minimum of 1 year prior to the study. This 9-month (96 workout) program was periodized into three,12-week mesocycles which included multi-set (3-5 sets) training with light intensity (12-15 repetitions with 60-90 seconds rest between sets), medium intensity (8-10 repetitions with 1-2 minutes rest between sets), high intensity (3-6 repetitions with 2-3 minutes rest between sets) and power (whole-body exercises at 30-45% 1RM with 3-min rest periods between sets). Exercises consisted of bench press, squats, hang cleans, biceps curls, heel raises, abdominal exercises, latissimus dorsi pulldowns, lunges, upright rows, push presses and weight plate lifts. Participants did the same training sessions but were divided into 3 groups, each with a different supplementation (whey protein, soy protein and carbohydrate) during the 9 months. Interestingly, and encouragingly, RMR increased in all female and male participants by approximately 5%. Unpredictably, there were no group differences in RMR increases due to the supplementation. In a most unique study design, Greer and colleagues (2015) measured E.P.O.C. after three energy expenditure matched workouts: RT (60% of 1RM to fatigue on seated pectoral flyes, squats, latissimus pulldowns, cable triceps push downs, and heel raises performed in a circuit (with 1 minute rest between sets) that was repeated over a 45-minute time period); moderate intensity steady state aerobic training at approximately 39% aerobic capacity which stopped when participant expended the same amount of calories as the RT workout; and HIIT training (30 seconds at 90% aerobic capacity followed by 120-180 relief at a light intensity) until the participants caloric expenditure of the workout matched the RT workout. There was no difference in the RT and HIIT E.P.O.C. values at 12 and 21 hours after the workouts. However both RT and HIIT E.P.O.C. values were significantly higher then the steady state aerobic trial. The RT E.P.O.C. values were 15% above baseline values at 12 hours and 12% above baseline at 21 hours. In practical terms, Greer et al. calculated that the increase energy expenditure from E.P.O.C to be approximately (and impressively) 300 additional calories over a period of 24 hours, as compared to the steady state aerobics bout. How Does RT Effect RMR and E.P.O.C. In regards to changes in RMR, Aristizabal et al. (2015) explain that muscle mass and thyroid hormones have a profound effect on RMR. The authors continue that resistance training prominently can lead to positive increases in muscle mass and it is possible that metabolic changes in muscle (from RT) may also influence thyroid hormones, though more research is needed in this area. With RT and E.P.O.C., Greer et al. (2015) summarize research that shows RT creates a higher degree of muscle damage than aerobic training, and the muscle protein repair/synthesis process is an expensive, energy demanding metabolic process (i.e., increasing caloric expenditure. Green and colleagues continue to explain that higher exercise intensities, regardless of mode, produce higher E.P.O.C. values. Practical recommendations When seeking improvements in RMR, the study by Aristizabal et al. (2015) clearly shows that periodized programs, with progressive cycling of various aspects of a training program with systematic changes in intensity and volume are a solid choice. To maximize E.P.O.C., performing compound exercises, that recruit the most amount of muscle mass, at higher intensities, relative to a person's fitness level is a very good strategy. Obesity Background Obesity (i.e. BMI > 30 kg/m2) is a chronic disease that ails 39.8% of Americans (93.3 million) and is higher (42.8%) among middle-aged (40-59 yrs) adults (Hales et al, 2017). The prevalence of obesity in youth 6-11 years is 18.4% and in adolescents 12-19 years it is 20.6% (Hales et al). Commonly, people attempt to lose weight with a blend of dieting, exercise, and treatment from various health-care professionals. RT is a potent stimulus that improves body composition by increasing muscle (i.e. lean body mass) while also decreasing fat mass concurrently (Strasser and Schobersberger , 2011). Research on Resistance Training in Obese Populations In their review of literature, Strasser and Schobersberger (2011) summarize that a significant number of studies have shown that RT is associated with a decrease in fat mass with a simultaneous increase in muscle mass. The authors continue that muscle mass increases are typically a minimum of 2 to 5 lbs. Strasser and Schobersberger also report that many studies also show that RT programs reduce visceral fat (i.e. fat stored around internal organs such as the liver, pancreas and intestines), also referred to as central obesity. Visceral fat is associated with the development of abnormal cholesterol, hypertension, insulin resistance, type 2 diabetes, and cardiovascular disease (Strasser and Schobersberger). How Does RT Promote Fat Loss Resistance exercise exposes muscle cells to a unique blend of metabolic stress, mechanical tension, and exercise damage, which converge on a variety of signaling mechanisms that increase muscle protein synthesis. When repeated over the course of weeks and months, acute increases in muscle protein synthesis results in increased muscle mass. Subsequently, the chronic accretion of muscle will increase gradually increase RMR (as discussed previously) and thus help facilitate weight loss. Practical recommendations Fortunately, there are a variety of different types of RT that have been shown to increase muscle mass, which is key to facilitating fat loss, improve body composition and lower the risks of obesity. Recently, RT research shows that exercise training volume, defined as sets x reps x load is a critical factor in improving muscle mass (Schoenfeld, Ogborn and Krieger, 2016), Schoenfeld and colleagues summarize there is a clear dose-response relationship between number of sets and hypertrophy. When counting weekly sets per muscle group, significant hypertrophy occurs with <5 sets (+5.4%), 5-9 sets (+6.5%), and >10 sets (+9.6%). Because hypertrophy occurs along a spectrum (i.e. 4-10+ sets), personal trainers have freedom to adjust training programs to fit their client's preference and current fitness levels. High Cholesterol Background According to the CDC (2019), in 2015-2016, more than 18% of adults 20 or older had high-density lipoprotein (HDL, or the “good”) cholesterol levels less than 40 mg/dL, while greater that 12% of adults had total cholesterol higher than 240 mg/dL. Essentially, CDC data indicate that 95 million U.S. adults age 20 or older have total cholesterol levels higher than the recommended 200 mg/dL (or lower) level. The CDC data woefully show that 7% of U.S. youth ages 6 to 19 have high total cholesterol. High blood cholesterol raises the risk for stroke and heart disease (CDC). The CDC recommends that healthy adults should have their cholesterol checked every 4 to 6 years. Those with heart disease or diabetes or who have a family history of high cholesterol, need to get their cholesterol checked more often. Research on RT and Cholesterol Fahlman et al. (2002) compared the effect of RT vs. AT on blood lipid profiles in 45 healthy, active women (age 70-87), who did not abnormal cholesterol levels. RT was performed 3 days/week and consisted of total body exercises for 3 sets of 8 repetitions to momentary muscular fatigue (could not do 9 repetitions) which was adjusted weekly during the 10 weeks of training. There was 2 minutes of rest between sets. The exercises, all lower body, consisted of 3 sets of leg extension, leg curl, plantar flexion, and dorsi flexion; two sets of hip flexion and hip extension; and one set of hip adduction and hip abduction. After 10 weeks, participants in the resistance training group decreased total cholesterol (-10mg/dl), LDL-C (-18.3 mg/dL), and blood fats (-29 mg/dL), with a positive increase in the 'good' HDL-C (+10.3 mg/dL). Strasser and Schobersberger (2011) emphasize that there is a paucity of research investigating the independent effect of RT on cholesterol in persons with abnormal cholesterol levels. Much more research is needed with men and women in this area. Practical Application An excellent review published by Mann and colleagues (2014), in which they summarize the effects of aerobic training, RT, and combined (RT and aerobic training) on blood lipid profiles. The researchers conclude that with RT and cholesterol changes, the data consistently show that programs with increased volume (i.e., reps x sets x load) have a greater impact on improving cholesterol profiles as compared to programs with increased intensity. In addition, from the review by Mann et al. there seems to be a synergistic effect from blending aerobic training and RT into a training program for optimal improvements in cholesterol profiles in men and women. Side Bar 1. Can Resistance Training Improve Cardiorespiratory Fitness? Maximal oxygen consumption (VO2max), the maximal rate that oxygen is consumed, distributed, and used for energy during exercise, is the most common measurement of cardiorespiatory fitness. Improving VO2max is important, as it is a powerful predictor of all-cause mortality for people of all ages and gender, regardless of pre-existing health conditions. Recently, researchers have looked closely at RT as an alternative means to improve cardiovascular fitness. Munoz-Martinez et al. (2017) conducted a systematic review and meta-analysis on circuit-based training programs that improve VO2max. From their research the authors summarize that programs need to include 14-30 sessions for 6-12 weeks, with each session lasting at least 20-30 minutes. All exercises are performed at intensities between 60% and 90% one-repetition maximum. Furthermore, each session should consist of 6-12 exercises per sessions, performing 12-15 repetitions or 20-40 s of work per station, and completing at least two circuits. Interestingly, Munoz-Martinez et al. highlight that resistance circuit-based training can greatly increase VO2max by 9.7%, which is remarkably noteworthy. There are many (many) unique training ways to design circuit RT as a cardiorespiratory stimulus. Personal trainers are empowered to be creative (and think outside the box) while staying within the guidelines of the established evidence. Conclusion In summary, the playbook is wide open, and personal trainers are limited only by their creativity and imagination. We encourage all fitness pros to use a variety of RT training modalities (i.e. free weights, suspension training, battle ropes, kettle bells, etc.) to build dynamic, fun, and engaging RT programs that best fit their client's goals and needs. Increasing muscle size and strength has numerous positive implications, including reduced blood pressure, improved insulin sensitivity, better lipid profiles, lower cholesterol, and improved body composition. The message is clear: lift weights, build muscle, and improve your quality of life. With every rep, we all get stronger! |
||||||||
 |
||||||||
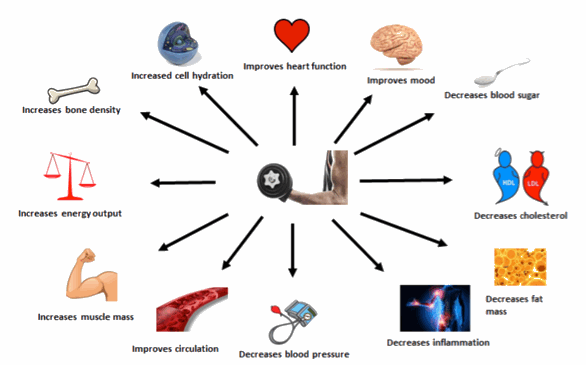
| Figure 1. Metabolic and Health Benefits of Resistance Training Data from Westcott, 2016 and Strasser, B. & Schobersberger, 2011 Bios: Zachary Mang, M.S. is a youth baseball coach in Albuquerque, NM and a doctoral student in Exercise Science at the University of New Mexico (UNM). His research interests include metabolic adaptations to HIIT, resistance training interventions in obese youth populations, and molecular adaptations to exercise as they pertain to health and fitness. Amber L. Logan is an Exercise Science student at UNM who's research interests include exercise for clinical populations and disease prevention as well as physical therapy rehabilitation for neurological populations. Fabiano T. Amorim, PhD. is a exercise physiology scientist at UNM who's research interests are insulin sensitivity in obese populations and exercise adaptations in the heat. Len Kravitz, PhD, CSCS is the program coordinator of exercise science and a researcher at the University of New Mexico where he received the Presidential Award of Distinction and the Outstanding Teacher of the Year award. References: AHA, 2017. The Facts about High Blood Pressure https://www.heart.org/en/health-topics/high-blood-pressure/the-facts-about-high-blood-pressure Retrieved January 24, 2019 Aristizabal, J.C., Freidenreich, D.J., Volk, B.M., et al. (2015). Effect of resistance training on resting metabolic rate and its estimation by dual-energy X-ray absorptiometry metabolic map. European Journal of Clinical Nutrition, 69, 831-836. Beck, D.T., Casey, D.P., Martin, J.S., et al. (2013). Exercise training improves endothelial function in young pre-hypertensives. Experimental Biology and Medicine, 238(4), 433-441. Bweir, S., Al-Jarrah, M., Almalty, A-M., et al. (2009). Resistance exercise training lowers HbA1c more than aerobic training in adults with type 2 diabetes. Diabetology & Metabolic Syndrome, doi:10.1186/1758-5996-1-27 Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2017. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services; 2017 Cornelissen, V.A. and Smart, N.A. (2013). Exercise training for blood pressure: a systematic review and meta-analysis. Journal of the American Heart Association, doi: 10.1161/JAHA.112.004473 Centers for Disease Control and Prevention. (2019). High Cholesterol Facts https://www.cdc.gov/cholesterol/facts.htm Accessed February 8, 2019 de Sousa E.C., Abrahin, O., Ferreira, A.L.L, et al. (2017). Resistance training alone reduces systolic and diastolic blood pressure in prehypertensive and hypertensive individuals: meta-analysis. Hypertension Research ; doi:10.1038/hr.2017.69 Fahlman, M.M., Boardley, D., Lambert, C.P., et al. (2002). Effects of endurance training and resistance training on plasma lipoprotein profiles in elderly women. Journal of Gerontology, 57(2), 54-60. Hales C.M., Carroll, M.D., Fryar, C.D., et al. (2017). Prevalence of obesity among adults and youth: United States, 2015-2016. NCHS Data Brief, 288, 1-8. Holten, M.K., Zacho, M., Gaster, M. et al. (2004). Strength training increases insulin-mediated glucose uptake, GLUT-4 content, and insulin signaling in skeletal muscle in patients with type 2 diabetes. Diabetes, 53, 294-305. Mann, S., Beedie, C., and Jimenez, A. (2014). Differential effects of aerobic exercise, resistance training, and combined exercise modalities on cholesterol and lipid profile. Sports Medicine, 44, 211-221. Mozaffarian, D., Benjamin, E.J., Go, A.S., et al. (2015). Heart disease and stroke statistics-2015 update: a report from the American Heart Association. Circulation, 131, e29-e322. Munoz-Martinez, F.A., Rubio-Arias, J.A., Ramos-Campo, D.J. et al. (2017). Effectiveness of resistance circuit-based training for maximum oxygen uptake and upper-body one-repetition maximum improvements: a systematic review and meta-analysis. Sports Medicine, DOI 10.1007/s40279-017-0773-4 Olson, T.P., Dengel, D.R., Leon, A.S. et al. (2006). Moderate resistance training and vascular health in overweight women. Medicine and Science in Sports and Exercise, 38(9), 1558-1564. Piras, A., Persiani, M., Damiani, N., et al. (2015). Peripheral heart action training as a valid substitute to high intensity interval training to improve resting cardiovascular changes and autonomic adaptation. European Journal of Applied Physiology, 115, 763-773. Schoenfeld, B.J. Ogborn, D.I., and Krieger, J.W. (2016). Dose-response relationship between weekly resistance training volume and increases in muscle mass: a systematic review and meta-analysis. Journal of Sports Sciences, 35(11), 1073-1082. Strasser, B. & Schobersberger, W. (2011). Evidence for resistance training as a treatment therapy in obesity. Journal of Obesity, doi:10.1155/2011/482564, 9 pages Westcott W.L., Winett R.A., Annesi J.J., et al. (2009). Prescribing physical activity: applying the ACSM protocols for exercise type, intensity, and duration across 3 training frequencies. The Physician and Sports Medicine. 37(2), 51-58. Westcott, W.L. (2015). Build muscle, improve health: Benefits associated with resistance exercise. ACSM's Health & Fitness Journal, 19(4), 22-27. Yavari, A., Najafipoor, F., Aliasgarzadeh, A. et al. (2012). Effect of aerobic exercise, resistance exercise, or combined training on glycemic control and cardiovascular risk factors in patients with type 2 diabetes. Biology of Sport, 29(2), 135-143. |
||||||||
|
|
||||||||
|