Sress Physiology: Understanding and Counteracting a Health Crisis
By Thea M. Benally and Len Kravitz, PhD
Introduction: Stress is Acute and Chronic
Stress is a widespread, growing health crisis across much of the world. The COVID-19 pandemic has seriously affected the mental and physical health of many client lives, disrupting work, health care services, classroom learning for students (of all ages), the economy and relationships (See Figure 1). According to Gulzhaina et al. (2018), stress is the process by which a person reacts when faced with internal or external challenges and problems. Rohleder (2019) synthesizes several studies indicating that in most cases, acute (i.e., short-term) stressors are beneficial for immediate survival. With acute stressors, a person often experiences the alarm reaction known as the 'fight or flight' response in which hormonal resources (i.e., adrenaline and noradrenaline) are mobilized (See Figure 2) (Anghelescu et al., 2018). Harkness and Monroe (2016) add that acute life stressors can vary in severity, or threat.
Chronic, or long-term stressors, are distinct from acute life events in terms of their ongoing and enduring nature (Harkness and Monroe, 2016). Physiologically, they are different from acute stressors (See Figure 2). Examples of chronic stressors, which also vary in severity, include dealing with an unending illness or prolonged financial difficulties. Rohleder (2019) summarizes evidence denoting that chronic stressors are associated with a large range of diseases, including cancer, insulin insensitivity, cardiovascular disease, as well as psychological stress responses (e.g. anger and anxiety) (See Figure 3).
|
 |
Figure 1. Stress in America: Key Findings From The American Psychological Association Report on the Pandemic
Source: APA, 2021.
|
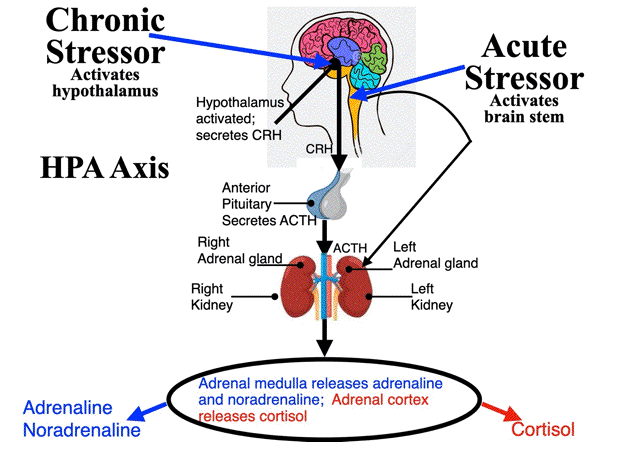 |
Figure 2. Physiological Origins of an Acute and Chronic Stressor in the Brain
Acute Stressor: Autonomic Nervous System Activation
The acute stressor activates the autonomic nervous system in the brain stem, which sends a message to the adrenal medulla to release the fight or flight hormones: adrenaline and noradrenaline
Chronic Stressor: Hypothalamic-Pituitary-Adrenal (HPA) axis
1) A chronic stressor activates the hypothalamus which releases corticotropin-releasing hormone (CRH), which activates to the pituitary gland
2) The pituitary gland releases adrenocorticotrophic hormone (ACTH), which activates the adrenal glands
3) The adrenal cortex releases glucocorticoids (GC); the dominant GC in humans is cortisol
4) There are cortisol receptors in the brain and most tissues in the body that regulate immune function, reproduction, cardiovascular function, metabolism and cognition
Sources: Gulzhaina et al., 2018, Azuma et al., 2018, Anghelescu et al., 2018
|
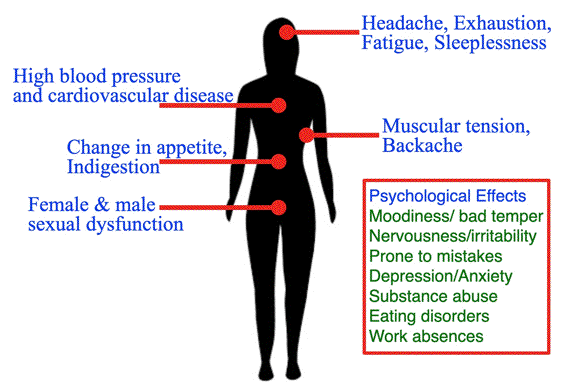 |
Figure 3. Physiological and Psychological Effects of Harmful Stress
Source: Adapted from Anghelescu et al., 2018
|
How Does Stress Impact Memory and Emotion Processing?
In a recent review, Lupiena and colleagues (2018) explain that enduring chronic stressors can contribute to the development (or continuance) of health problems, due to elevated glucocorticoid hormones, particularly cortisol. When cortisol levels are elevated, they can directly access and impact cognitive processes in the brain, leading to impairments in attention, memory and emotion processing. Areas of the brain affected by elevated cortisol are the prefrontal cortex, the hippocampus, and the amygdala. Lupiena et al. expound that these three brain structures play a crucial role in the interpretation of a situation as being stressful, and in the subsequent selection and inhibition of possible responses. The researchers also note that chronic, elevated production of glucocordicoids are also highly associated with the development of depressive disorders.
How Does Stress Increase a Person's Risk for Heart Disease?
Chronic stress has a high risk for multiple types of cardiovascular disease (Song et al., 2019). However, until most recently the mechanism how stress translates to cardiovascular disease has been unknown. In a landmark study by Tawakol et al. (2017), the researchers showed (for the first time) that there is a definite mechanism linking cardiovascular events with resting metabolic activity within the amygdala (in the brain), which was preceded and brought about by arterial inflammation.
A Fitness Professional's Toolbox for Helping Clients Manage Stress
It is important for fitness pros to share with clients that stress is a reality of everyday life (Gulzhaina et al., 2018). Stress management interventions use mind-to-body and body-to-mind strategies (See Figure 4) to reduce the effects of chronic stress (Fish, 2018). Interestingly, for clients who enjoy taking yoga classes, a recent study showed that practicing yoga at the local gym twice a week effectively improves psychological health for the general working public (Maddux, Daukantaite, & Tellhed 2018).
Here are 4 evidence-based stress management interventions fitness pros can teach their clients.
Mindfulness Meditation: Meditation is an intervention where a person sits comfortably for several minutes (20 to 40 minutes) and focuses on her/his internal breathing. It has been shown to reduce stress, negative emotions, anxiety and depression and strengthen areas of the brain associated with relaxation and joy (Gulzhaina et al., 2018). With mindfulness meditation, have the client laser focus on the present moment, not dwelling on the past or trying to imagine what's in the future. Encourage the client not to overanalyze, judge or overthink the stressful situation.
Diaphragmatic Breathing: Diaphragmatic breathing (also known as abdominal or belly breathing), is a stress intervention that can help lesson a stressor, lower high blood pressure and decrease anxiety and depression (Fish, 2018). Fish highlights when clients become stressed, they often lift their shoulders to inhale and exhale and their breath becomes short and shallow, which if sustained, may actually intensify the stressor. With diaphragmatic breathing, have clients perform slow, even, deep breathing through the nose, for 5 to 10 minutes (progressing to 15 to 20 minutes), while engaging the diaphragm (on the inhalation). When the diaphragm is engaged (i.e., lowers into the abdominal cavity), the belly will protrude (easily observed by placing a hand on the abdomen) on the inhalation, and there is minimal shoulder and chest movement.
Progressive Muscle Relaxation: Progressive muscle relaxation is an effective intervention for reducing stress and anxiety, by consecutively tensing and relaxing the muscles (Gulzhaina et al., 2018). The muscle groups to tense and relax can be the feet, legs, buttocks, abdomen, chest, shoulders, arms, hands, forehead and face. In a sequential pattern (such as from feet to face), have a client close their eyes, and purposely contact a muscle group (near maximally while breathing in) for 10 seconds and then relax the contraction for 20 seconds (while slowly exhaling). Then go to the next muscle group and repeat the contraction/relaxation cyle. It helps to instruct each client to focus on the muscles contracting and relaxing, so she/he learns the distinct difference in tension and relaxation with the muscles. Progressive muscle relaxation has been shown to reduce cortisol levels, high blood pressure, headaches, and improve cardiac management of patients after bypass surgery (Gulzhaina et al., 2018).
Positive Mental Imagery: Mental imagery is recognized in research as an important intervention for mental health treatment of stress, anxiety and insomnia (Jerath et al., 2019). Positive mental imagery, which is imagining a nice place, is cost effective and can readily be used at home. Visualizing beautiful scenes (5 to 15 minutes) may also improve the quality of life for a client (Jerath et al.). Jerath et al. discuss research that shows that natural environments (such as a forest atmosphere) form a deep connection with nature. The researchers submit that targeting stress arousal when it is time to sleep is optimal because it promotes relaxation.
|
 |
|
Figure 4: Exercise Combats Stress in Several Ways
Sources: Ochentel, Humphrey, and Pfeifer 2018; Jackson, 2013
|
 |
Side Bar 1. 10 Holiday Stress Coping Strategies
With the holidays often comes new stressors for clients. Family get togethers, shopping, decorating, gift buying and wrapping, cooking and baking, and attending special activities can place extra demands on clients and lead to stress.
Here are 10 holiday stress coping strategies from the Mayo Clinic ( 2020).
1) Reach out: if you feel lonely or isolated, seek out community, religious or other social communities
2) Be realistic: even though your holiday plans may look different due to the pandemic and other issues, you can find ways to celebrate
3) Acknowledge your feelings: it's normal to feel multiple feelings including sadness, grief and happiness during the holidays
4) Take a break for yourself: find an activity that clears your mind
5) Keep up your health habits: eat healthy meals, get plenty of sleep, maintain your regular exercise routine, and take a breather from technology
6) Be budget savvy: decide how much money you can afford to spend on gifts and food and stick to it
7) Plan ahead: good planning helps to combat last-minute scrambling
8) Lean to say no: friends and colleagues will understand if you can't participate in every activity
9) Take control: recognize your holiday triggers, such as financial pressures, so you can prevent them
10) Get help if you need it: if you feel persistently irritable, hopeless, or sad, and unable to face your daily routine, talk to a mental health professional.
Conclusion
Fitness pros have an incredibly meaningful opportunity to help clients deal with mounting life stressors. The stress management strategies presented in this article are effective, evidence-based, require no specialized equipment, and are easily introduced by fitness pros to clients. Begin the de-stressing, now!
Author Bios:
Thea M. Benally is completing her B.S. in Exercise Science with a minor in Population Health at the University of New Mexico. Her research interests include exercise for clinical populations, physical therapy rehabilitation for patients with cardiovascular disease, and endocrinology research specifically in American Indian populations.
Len Kravitz, PhD, CSCS is the program coordinator and professor of exercise science at the University of New Mexico where he recently received the Presidential Award of Distinction and the Outstanding Teacher of the Year award. In 2016 Len was inducted into the National Fitness Hall of Fame.
References:
Anghelescu, I-G., Edwards, D., Seifritz, E. et al. (2018). Stress management and the role of Rhodiola rosea: a review. International Journal of Psychiatry in Clinical Practice, 22(4), 242-252.
Azuma, K., Zhou, Q., Niwa, M. et al. (2017). Association between mastication, the hippocampus, and the HPA Axis: A comprehensive review. International Journal of Molecular Sciences, 18, 1687; doi:10.3390/ijms18081687 (14 pages)
Fish, M. T. (2018). Don't stress about it: A primer on stress and applications for evidence-based stress management interventions in the recreational therapy setting. Therapeutic Recreation Journal, 52(4), 390-409.
Gulzhaina, K.K., Aigerim, K.N., Ospan, S.S., et al. (2018). Stress management techniques for students. Advances in Social Science, Education and Humanities Research, 198, 47-56.
Harkness, K.L. and Monroe, S.M. (2016). The assessment and measurement of adult life stress: Basic premises, operational principles, and design requirements. Journal of Abnormal Psychology, 125(5), 727-745.
Jerath, R., Beveridge, C. Jensen, M. et al. (2020). The therapeutic role of guided mental imagery in treating stress and insomnia: A neuropsychological perspective. Open Journal of Medical Psychology, 9, 21-39.
Lupiena, S.J., Justera, R-P, Raymonda, C. et al. (2018). The effects of chronic stress on the human brain: From neurotoxicity, to vulnerability, to opportunity. Frontiers in Neuroendocrinology, 49, 91-105.
Maddux, R.E., Daukantaite, D., and Tellhed, U. (2018). The effects of yoga on stress and psychological health among employees: an 8- and 16-week intervention study. Anxiety, Stress, & Coping, 31(2), 121-134.
Mayo Clinic. (2020). Stress, depression and the holidays: Tips for coping.
https://www.mayoclinic.org/healthy-lifestyle/stress-management/in-depth/stress/art-20047544
Ochentel, O., Humphrey, C., and Pfeifer, K. (2018). Efficacy of Exercise Therapy in Persons with Burnout. A Systematic Review and Meta-Analysis. Journal of Sports Science and Medicine. 17, 475-484.
Rohleder, N. (2019). Stress and inflammation - The need to address the gap in the transition between acute and chronic stress effects. Psychoneuroendocrinolog, 105, 164-171.
Song, H., Fang, F., Arnberg, F.K., et al. (2019). Stress related disorders and risk of cardiovascular disease: Population based, sibling controlled cohort study. British Medical Journal, 365, l1255.
Tawakol, A., Ishai, A., Takx, R.A.P. et al. (2017).Relation between resting amygdalar activity and cardiovascular events: a longitudinal and cohort study, The Lancet, 389, 25 February-3 March 2017, 834-845.
End
|
|
|