|
|
| Metabolic Adaptations What does RER stand for? How is it determined (ratio: VCO2/VO2)? What are the theoretical endpoints of the RER? What is VO2 max? What are the criteria to know it has been achieved—can you list them all? What is the average improvement (in untrained persons) seen with VO2max from training? How do we describe plateau in VO2? How long should a VO2 max test be? What is VO2 peak? What is the difference in VO2max and VO2 peak? Absolute (L O2/min) and relative (ml O2/kg/min) are two ways of expressing VO2? Which is better for comparison of individuals and why? QUESTION ON 'FAT BURNING': If a FIT person wished to optimize ‘Fat Burning’ and has only 30 minutes to do the actual aerobic portion of the workout (warm-up and cool-down are separate), how would you recommend they exercise? Answer = COMFORTABLE but CHALLENGING pace. Remember the two “C” words (COMFORTABLE but CHALLENGING). Recommend that the person train at a Comfortable but Challenging pace they can sustain to burn more calories! In essence, to BURN more FAT a person should attempt to BURN more calories. One more time: To burn more fat, a person needs to BURN MORE CALORIES! CLASS, IF O2 DEFICIT AND EPOC ARE NOT COVERED IN THIS UNIT, THEY WILL BE IN THE NEXT UNIT. ONLY WILL TEST IF WE COVER THEM IN CLASS. What is O2 deficit? What is EPOC and name at least 5 factors that contribute to it? Class, CLICK HERE for a LINK that explains O2 deficit and EPOC. Adaptations to Aerobic Exercise With aerobic training do the slow-twitch fibers actually show some hypertrophy (how much)? A key adaptation of aerobic training is capillary supply. How much of an increase may be seen? If the capillaries increase is in number, how does this affect O2, delivery? What does myoglobin do? What fiber, Type I or Type II is high in myoglobin? How much may myoglobin increase with aerobic training? Mitochondria function is proposed to improve with aerobic training? What happens to the size and number of mitochondrion with aerobic training?). How much does research show that oxidative enzymes may increase due to aerobic training? Aerobically trained muscle can oxidize fatty acids better. How much is this increased ability (what %)? If you are able to utilize fat more efficiently, in the long run how will this effect glycogen depletion? Metabolic Adaptations to Anaerobic Exercise Adaptations of phosphagen energy system. With very short burst training what adaptations do we see to the phosphagen system? (note, it improves but it is currently debatable how much this improvement is) The glycolytic training is optimized with high-intensity short bout exercise up to 1.5 minutes. 30-second training bouts (perhaps in an interval training format) have been shown to increase what enzymes of the glycolytic energy system? Explain how with glycolytic training, there is an increase in buffering capacity. What are the names of some buffers? What are they doing? The pH scale in a sense, tells you the concentration of what is in a solution (Answer: H+)? If the pH goes below 7 is the concentration more or less acidic? Is lactate really causing the acidosis or is it something else? What would this be? (It is the accumulatin of H+ from the hydroysis of ATP) CLASS: IF NOT COVERED IN THIS SECTION, THIS WILL BE ON A FUTURE EXAM! Fatigue Brief Essay (Please know!): In class, we broke down the sites of Peripheral Fatigue into 3 MAJOR areas (one at neuromuscular junction and two in the muscle. Explain them! Points to discuss include how are the protons affecting calcium binding to troponin; how do the protons affect ATPase; what happens at the neuromuscular junction?). Class, Click Here for a link that further explains Peripheral Fatigue. Make sure you know this. What depletes first, CP or ATP? Why? See below for answer. (CP deplets first: Remember, CP is replenished only by ATP. However, ATP is replenished by the phosphagen energy system, glycolysis, and mitochondrial respiration) |
||||||||
|
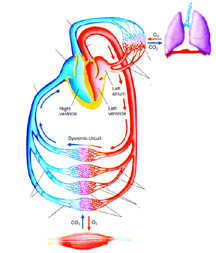
Cardiovascular Physiology The right side of the heart is associated with the pulmonary or systemic circuit. Self-test: Put this blood flow tracing in correct order starting with venules: Scroll Down to check your answers:
Trace very clearly the cardiac conduction system from the SA node, AV node, AV bundle, bundle branches, and purkinje fibers. Is the SA node in the right or left atrium? What is the ability of the heart to generate it’s own electrical signal called? (Answer: Pacemaker or autorhythmic) In actuality, when the ventricles pump, they must squeeze 1) from bottom up or 2) from top down? Describe the components of a EKG tracing including the P wave, QRS complex, and T wave. When is atrial depolarization and repolarization? When is ventricular depolarization and repolarization? Can you draw and explain this electrical event? What is normal sinus rhythm? What is sinus bradycardia? What is sinus tachycardia? What would a normal stroke volume be in ml/beat? What is end-diastolic volume (EDV) stand for? What is end-systolic volume (ESV) stand for? Mathematically how can you describe SV, EDV and ESV? Heart rate is always looked at in beats per ______? What is ejection fraction? An average ejection fraction would be what percent at rest? How would you classify an ejection fraction of 70%? How would you classify an ejection fraction of 50%? What does cardiac output represent? Is it liters per beat, per min or per hour? Mathematically, if you have two of the following you can always calculate the third (EDV, ESV, SV). Make sure you can do this. For instance, if EDV is 110 ml and SV is 55 ml, what is ESV. Or if ESV is 60 and SV is 65, what is EDV? Make sure you can calculate ejection fraction. What would be considered an average ejection fraction? Make sure you can calculate cardiac output in ml/min as well as L/min. Here are some practice calculations. Make sure you can do all of these! EDV = 110, SV = 70: What is ESV and What is Ejection fraction? ESV = 80, SV = 80: What is EDV and What is Ejection fraction? EDV =120, SV = 70: What is ESV and What is Ejection fraction? If HR = 180 b/min and SV = 100 ml/b what is Q? If HR =195 b/min and SV = 115 ml/b what is Q? Ventrical Volumes Solving practice: |
||||||||
 |
||||||||
| Answers to Blood Flow Quiz of Pulmonary and Systemic Circuit | ||||||||
|
||||||||
|